Stories
A New Approach to Dementia Care in Québec
In the next 15 years, nearly a million Canadians will be affected by Alzheimer’s or related disorders. Many of these people will end up living excluded from society. The nonprofit residence Carpe Diem is part of a movement to change how we view people with dementia.
Text—Eugénie Emond
Photos—Catherine Bernier
The scent of linden blossoms has overtaken that of pulp and paper in Trois-Rivières, Québec. All across the city, trees covered in flowers exude a heady scent.
Three women on a walk stop on each city block to swoon over the greenery. “Heavens, it’s beautiful! There isn’t even any trash!” exclaims Jocelyne. “I love when the trees kiss,” adds Denise, eyes glued to the leafy canopy above our heads. A neighbour waves as she weeds her garden, clearly accustomed to seeing them pass by.
Jocelyne’s ahead now. She looks back over her shoulder and proudly measures the growing space between her and the other women. A little further and she would have lost them. Jocelyne is a former head nurse who used to spend entire days on her feet. At 78, she’s still in great shape. Every day Jocelyne heads out, alone or with a few of the other residents, sometimes an attendant.


This is probably what is most striking about Carpe Diem, a home for people with Alzheimer’s and related disorders: the personal freedom accorded to residents.
In a society where safety, insurance, and civil liability issues tend to take precedence, Carpe Diem stands out. The non-profit residence houses 15 people and also offers home support. Here, those who are able can go on walks through the neighbourhood, take part in meal preparation, help with setting up the fire in the outdoor fireplace, and walk up and down the large staircase.
It’s an environment where the safety net is carefully hidden and the surrounding community is in the know.
As I walk with Jocelyne, I remember my former neighbour and his repeated visits to my house. He would sometimes show up with his empty bottles, thinking he was going to the general store, the one he used to know, back in the day. I had notified his family, thinking this elderly man would surely not be able to stay at home alone much longer. And what about driving the car? Would he find his way home? Would he cause an accident?
Soon after, I learned that he had moved out of the house where he had lived for most of his life. As I watch these three women taking a walk and notice my surprise at their (supervised) freedom, I realize the limits of my knowledge of the disease they face.
Redefining Alzheimer’s
—
Alzheimer’s—which is caused by the progressive degeneration of brain cells—is accompanied by a frightening vocabulary: dementia, wandering, running away, stealing . . . and that’s just the beginning.
“Behind the word ‘wandering,’ there is the notion of walking aimlessly, but who are we to say that these people have no aim when they are walking?” asks Charlotte Berjon, coordinator of Carpe Diem. “They have the same aims as we do: entertaining themselves, letting off steam, going to the bathroom, eating and drinking. Why do we change the words the moment there’s a diagnosis?”
The diagnosis is always received like a verdict: the moment everything changes.
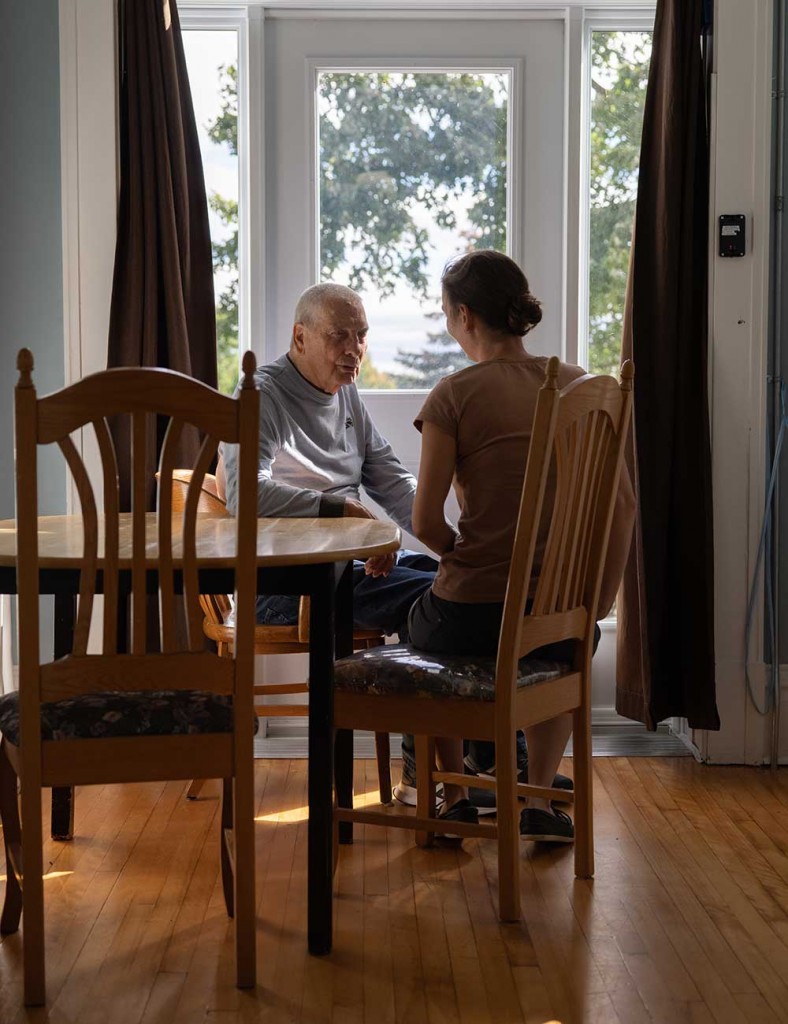

“The disease is viewed in a very dramatic way, because the image we have is of someone who is dying, about to disappear.”
Gloria Frisone, a doctor of social anthropology and ethnology at the École des Hautes Études en Sciences Sociales (EHESS) in Paris, has studied how loss of identity is connected with memory loss—and the significance of this in contemporary society.
“This link is anchored in our history of thought. It also relates to the conception of the soul: in our religious and philosophical culture, the soul is the essence of who we are, and therefore the death of the soul is even more shocking than the death of the body or the person. It’s something that goes against nature.”
Since the discovery of Alzheimer’s disease in 1906, things have changed greatly. This condition is no longer seen by researchers as relating only to the brain—something to be warded off with sudoku sessions.
Although it’s still fatal, studies published in 2020 in the Lancet identify a dozen risk factors and actions that can be taken to prevent it. According to Annette Leibing, medical anthropologist and professor in the Faculty of Nursing Sciences at the Université de Montréal, these new ways of understanding the condition have made for a “new dementia.”
“Modifiable” risk factors include type 2 diabetes, hypertension, smoking, social isolation, and air pollution. “In countries where there is very good access to health and education systems, the prevalence of the disease has lessened. There are more cases because the population is aging, but we can see that the numbers are decreasing.”
The professor adds that dementia has become a political matter. “If the numbers increase, it means that society has not done its job.”
New models for elderly care
—
On our way back from the walk, Madeline catches me glancing at the weather app on my phone. “Tomorrow’s another day!” she philosophizes. I put my device away and with it, my worries about a family weekend spent in the rain.
I observe the activities in the residence’s backyard: Madeline folding napkins and humming; Richard playing pétanque with a few roommates; Jocelyne carrying a tray of watermelon slices; Gaston with his eyes half-closed, a bright yellow marigold tucked in his buttonhole, letting himself be rocked by the gentle breeze.
On the balcony, an attendant helps Lise, who now spends her days in her adapted wheelchair, to eat her snack. No past, no future. Only the present, passing peacefully as dandelion seeds. Finally, a little respite, I think to myself.
“When people have memory problems, their capacity to project themselves forward and backward in time is limited. It’s here and now.”
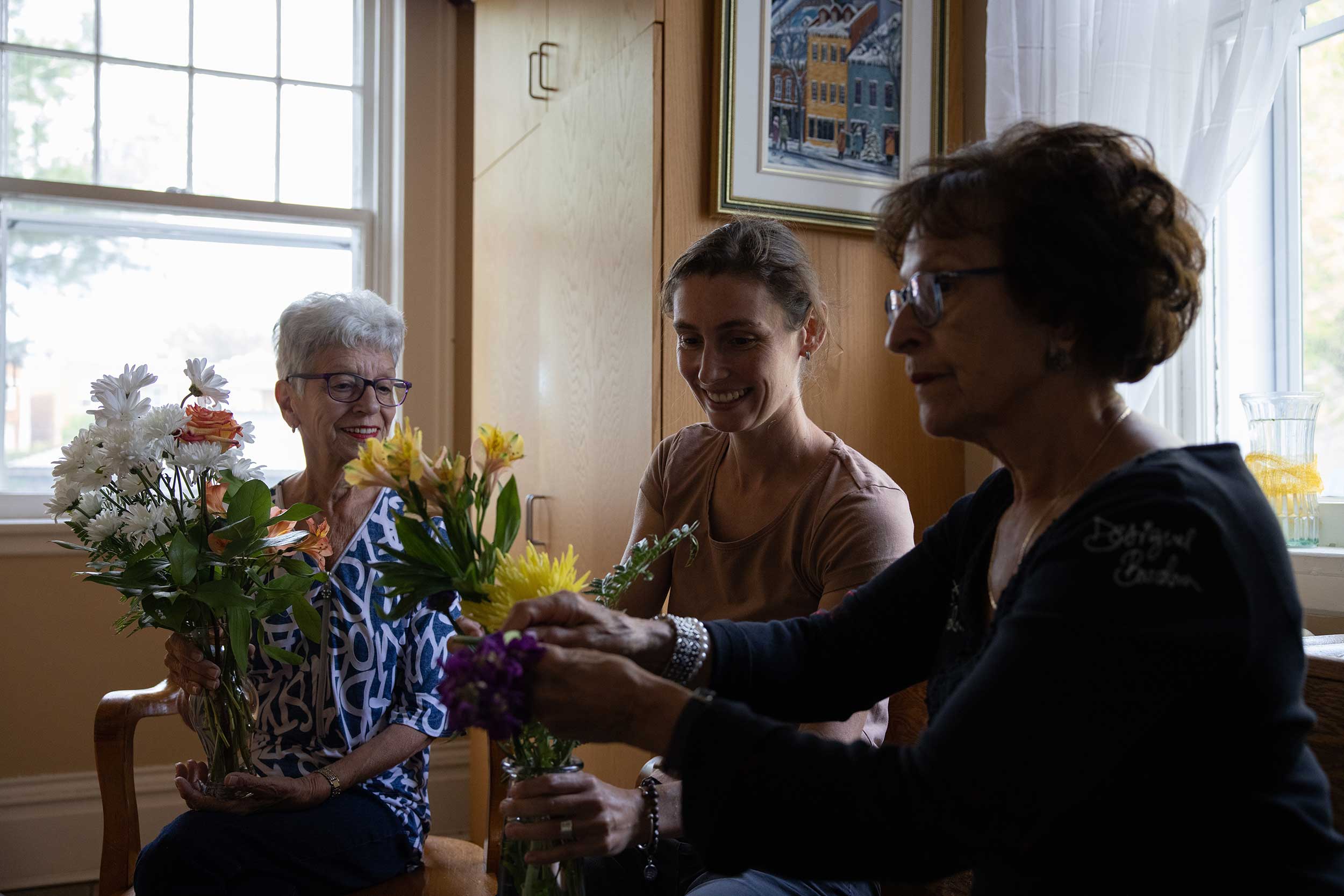
Charlotte Berjon, coordinator at Carpe Diem, accompagnied by residents Madeline and Jocelyne.
Philippe Voyer, a professor at the Faculty of Nursing Sciences at Université Laval, was inspired by Carpe Diem’s model when he participated in the creation of residences for elderly people in Québec—including the Humanitae complex in Québec City, and the provincial government’s seniors’ homes. These are intended to complete or replace the Long Term Care Home centres, where nearly 80 per cent of clients have been diagnosed with some form of cognitive disorder.
“We do everything we can to help these people experience positive emotions, which helps their mood remain positive as well,” he says.
Voyer is interested in the different care models emerging in Canada and the rest of the world. “Some of them place emphasis on the physical environment; others on the approach with residents,” he says. He mentions the Greenhouses in Nova Scotia and the United States, modest bungalows housing 6 to 12 people, a size that allows personnel to adapt their care routines for each person.
He also mentions Green Care Farms, where residents participate in a farm’s upkeep, a model developed in Holland that has gained traction throughout Europe. Animal sounds, the taste of garden vegetables, and the proximity of nature all work together to awaken the residents’ senses and “stimulate their residual capacities.”


The Carpe Diem model focuses on what residents have to offer at this moment in time; it respects their rhythm and seeks to understand the reason for certain behaviours before intervening. It’s a philosophy that requires staff and family members to anchor themselves in the present moment:
What do you do with a person who has cognitive impairment? What do you say? What do you share, when memories are erased?
Improving communication and quality of life
—
Over the phone, Pierre Martin tells me about his wife, Suzanne, who has had Alzheimer’s for more than six years. “I love her more than ever!” Martin has had to adjust his own approach during his daily visits to Carpe Diem in order to receive what his partner has to offer now.
“Our culture drives us forward and we focus so much on shared stories of the past. The pressure put on memory is enormous!” says Anne Basting, author and professor at the University of Wisconsin. She has developed a creative approach for patients, families, and caregivers to have meaningful relationships. Among other tools, she offers questions that don’t involve right or wrong answers (e.g., “What sounds do you hear?”) as keys for communication.
“Sometimes in dementia a caregiver is still in shock at what happens to the brain. They focus on repairing the losses when really all that does is lock you in the past and out of the present.”
Martin takes his wife out for drives in the car, and they sing songs together. The hardest thing now is not grieving what they used to be to each other, but handling the reactions of their kids. One of them finds it particularly difficult to see his mother in this state, and wishes “they would give her a needle and be done with it.” Martin tries to explain: “Please understand—it’s not because he doesn’t love her.”
As I listen to him, I realize that this conversation around the desire “to be done with it,” if the disease shows up, is becoming more and more common. It’s true that many have watched someone close to them experience major cognitive disorders or Alzheimer’s disease; some have been horrified by the slow agony, or by the quality of care their loved one received.
But for geriatrician and ethics researcher Félix Pageau, who wrote a manifesto about medically assisted death for people with mental disorders, the solution lies elsewhere.
“Patients with dementia are elderly, disabled, and often have associated problems of mobility and psychiatric issues. It’s a contempt for all this—into which we project ourselves—that causes us to say, ‘If I become like that, I don’t want to keep living.’ What I’m saying is, rather, that we should provide better care for these people, so they are as comfortable as possible in all these various states.”

Richard, resident of Carpe Diem.
Preserving identity beyond memory loss
—
In the backyard of Carpe Diem, Richard picks up a dishtowel to give Madeline a hand. Richard is 76 years old, with blue eyes that are nearly turquoise. He has the face of a Hollywood actor, with long lines etched across it. He tells me about the shock he felt upon receiving his diagnosis—of the feeling of abandonment he had when he left his home to move here six months ago. About how he still goes cycling every day. About the other residents. About their state, which is declining before his eyes. About what awaits him.
“What are you most afraid of?”
“The loss of my mental capacity.”
“Memory?”
“Memory is a lot of things. It’s not just one element dissociated from all the other mental faculties. It’s life habits, behavioural parameters, and emotional stability, I would say.”
This notion of memory, inseparable from Alzheimer’s disease, is a subject Gloria Frisone analyzed in her thesis in social anthropology. “Amnestic disorders and loss of memory are always cited first, even if they aren’t the only disorders that are part of the disease.”
Alzheimer’s can also affect behaviour, physical capacity, emotions, and cognitive functions. For example, people speak of semantic memory when someone can’t find the words any longer, “but this is actually a question of language impairment disguised as a memory issue,” says Frisone.
Speaking with Richard, you might imagine that the illness is not progressing.
“It’s deceptive, because the way the house is organized gives visitors the impression that residents don’t have very serious cases,”
And yet, no one here goes to the bathroom or bathes on their own. The more the disease progresses, the more constant is the care. Some residents are able to finish their days at Carpe Diem and receive adequate palliative care, but others must be transferred to a Long Term Care Facility (LTCF) when their state requires it.
Several people have ended up at Carpe Diem after being kicked out of their previous residences for behavioural problems—often because their care was poorly adapted to their condition. Here, in this former rectory in a residential neighbourhood in Trois-Rivières, they’re able to recover some of their dignity.
Social acceptance of cognitive decline
—
In the kitchen, Charlotte is wiping the table with an imaginary cloth, her movements firm and sure. Her vision has declined to 20 per cent. A constant whispering sound comes from her mouth: reminiscences, a few scraps of which can sometimes be heard—“must bring in the wood!” The attendant places a cloth in her hand, just in time for the last corner of the table.
“Carpe Diem maintains a certain degree of autonomy for people by drawing upon brain functions that existed 20 or 30 years before and which are still very active,” says Dr. Rémi Bouchard, a retired neuropsychologist and founder of the first memory clinic in Canada. “We rely heavily, for example, on procedural memory, that of the automatic gesture that’s been repeated thousands of times in a life,” adds Nicole Poirier.
Because episodic memory is affected, care at Carpe Diem often begins before residents even arrive. The same attendant who does home visits for a particular person will be the one to welcome them and work as their primary caregiver when they move into the residence. These recurrent meetings anchor themselves in the new resident’s memory and help to offset disorientation upon arrival. It’s a way of operating that requires a fair amount of flexibility and organization.
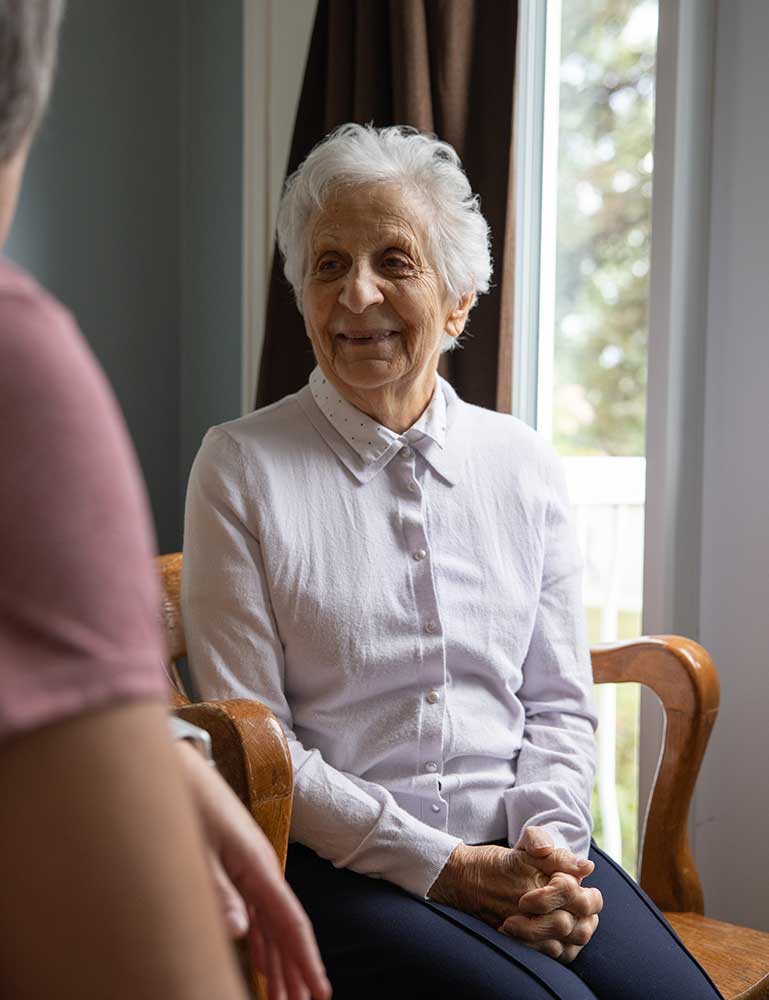
Poirier began to develop Carpe Diem in 1985, after directing a residence for elderly people for a few years and realizing the extent to which its services were maladapted for people with cognitive disorders. The road was long: she wanted an NGO that was accessible and financed by the government, and in 1995 she finally got it. Although there is a great deal of research showing the benefits of this kind of organization, the model has yet to really catch on here.
“At the MHSS [Ministry of Health and Social Services], they don’t have the ‘elderly people’ reflex. LTCFs have always been the poor relations at the Ministry of Health,” says Marguerite Blais, the provincial government Minister for Seniors and Caregivers, to account for the low level of innovation in terms of care for elderly people with cognitive disorders. The MHSS is in the process of constructing 48 seniors’ homes, smaller units that are partly inspired by what Carpe Diem is doing. The project has been accelerated by the pandemic, during which nearly 8,200 seniors have died of COVID-19 in LTCFs in Québec.
The construction of these houses has been criticized, however, because of the costs: some $2.4 billion for the whole project. Some would like to see more emphasis placed instead on home care, a change of tack that has been slow to materialize. Another priority is healthcare staff—of which there are not enough—who would benefit from being better trained in issues around major cognitive disorders.
The minister also notes that the public is generally ill-informed about Alzheimer’s disease.
“I’ve had people say, ‘It’s not important if the environment [Alzheimer’s patients live in] isn’t beautiful. They won’t even notice.’ Come on!”
These days the founder of Carpe Diem mainly gives training courses in Europe. When the first Alzheimer’s village was created in France, she was consulted. But she finds it unfortunate that these villages, which recreate a fictitious residential environment, enclose the patients rather than preserving their link to the surrounding community. Here, for example, the corner store is in the know: if a resident comes in unexpectedly for a bag of chips, the employees won’t make a big deal of it; they just put the amount on the house’s account.
The community’s involvement matters so much because Alzheimer’s carries its share of exclusion, combined with the spectre of a degenerative disease, which so many abhor. “The fear, which is so great in our Western world, comes from the fact that the disease weakens our thinking ability. In other countries this is less important,” says Annette Leibing, a medical anthropologist.
Leibing points to Brazil, where she used to teach, and where slight cognitive disorders tended to be quite well accepted. “When people showed symptoms such as wandering, it came with a high level of social exclusion, but if the person was gently starting to forget things, it was considered normal: slowly, the person was going to disappear and enter another world.”
“Elsewhere, there is far more acceptance—in China, India, or Japan, for example—of the fact that the elderly person at home is slowly losing their mental capacity. People speak about the disease much less. There’s not this vision of cognitive decline as pathological aging,” adds Frisone.
She notes, though, that in general, the biomedical point of view is accepted, “influenced by the historical opposition between the wise elder and the lunatic. Lunatics don’t have a social role anymore, because they can’t transmit the historic memory of their group.”
But those who spend time with people suffering from cognitive disorders recognize all they still have to offer. “They teach us how to live,” says Poirier unequivocally.
“If you pass one of them and don’t greet them, don’t look at them, they’ll hit the table. We call this behavioural problems, but it teaches us to enter in a real way into relationships with others. And this applies to all spheres of life.”
Pageau goes a step further. “Patients with dementia remind us of our own fragility in a North American society built around productivity. We value autonomy and functionality, but everyone has fragilities to varying degrees; why, then, would we not try to see how these people could help us to slow down, to take the time to live, rather than always racing toward our death?”
Balancing past and present
—


A melody drifts from the living room; an attendant has taken out her violin. Her bow keeps time, little by little involving Charlotte’s feet, which lift her up, moved by the traditional music. Back straight, arms lifted, she bows her head and greets the audience with a theatrical gesture, innate—like she did way back when she and her husband were a star ballroom couple. Richard moves forward and takes her in his arms, his blue eyes gazing deep into hers.
The day before, while Richard was setting up the fire, I asked the former criminologist if it was possible for us to exist without our past.
“Yes. Absolutely, but we have to continue to develop our identity here.”
“And what is our identity?”
“It’s our past, our present, and what we’re projecting into the future.”
“In spite of the disease, people still have all that?”
“Yes, because we retain our emotional dimensions for the most part. When I experience something I always try to attach an emotional cord so it will stick, so it will stay in my memory. I didn’t use to place any importance on that. But now I do.”
The sound of the gate closing startles us. The walkers are returning, perked up by their latest excursion. Madeline heads toward the laundry basket, determined to get through it. Nearby, three men take a leisurely sun bath. As I observe this uneven division of tasks, I think to myself: It’s true, we don’t ever completely forget what we’ve been.
Note: Residents are referred to by their first names only for the purposes of this article. Carpe Diem’s approach, however, supports the use of people’s full names.
Eugénie Emond is an independent journalist. She is also finishing her master’s in gerontology at the University of Sherbrooke. This year, her work was awarded two Grand Prizes for independent journalism and a gold medal at the Digital Publishing Awards. Website / Instagram
Catherine Bernier is a creative director, a freelance writer and photographer, and co-founder of The Parcelles, a seaside retreat for artists in residence in Nova Scotia. The influence of nature and culture on human choices and stories remains one of her core interests. Instagram / LinkedIn
Never Miss Another Issue
Two issues per year
25% OFF previous issues
Free Shipping in Canada